What exactly is platelet-rich plasma?
PRP injections offer ways to heal the body naturally - a feat made possible by platelet-rich plasma.
PRP has become very popular over the last decade.
But what exactly is platelet-rich plasma?
Platelet-rich plasma is a product made from a person's blood. A blood sample with PRP tubes is centrifuged in a PRP centrifuge to increase the concentration of platelets in the plasma. The result is a super-rich plasma with a platelet concentration of 94% compared to 6% normally found in human blood.
How platelets heal the body
Among other things, the plasma contains certain substances that are responsible for wound healing, the so-called growth factors. Together they form a complex system that is immediately activated in the event of injury and ensures the fastest possible regeneration. With this healing power, the body protects itself very effectively.
A typical blood sample consists of 93% red blood cells, 6% platelets and 1% white blood cells .
Platelets were first seen in blood in 1842 by the French doctor Alfred Donné. These are small disc-shaped cells with a lifespan of about 7 to 10 days.
After an injury that causes bleeding, platelets are activated and aggregate to release their granules, which contain growth factors that stimulate the inflammatory cascade and the healing process. Platelets are responsible for haemostasis, building new connective tissue and revascularisation, and most of the research in the last century has focused on this major function.
Only in the last two decades have we learned that platelet activation releases healing proteins in the body called growth factors.
There are numerous growth factors with different functions, but cumulatively they can accelerate the healing of tissues and wounds.
The ideology behind PRP treatment is to reverse the ratio of red blood cells to platelets by reducing red blood cells to 5% (which are less useful in the healing process) and, more importantly, concentrating platelets, which contain a potent mixture of growth factors, to 94%.
A normal platelet count in a healthy person is between 150,000 and 450,000 cells per microlitre of blood. Platelet concentrations of less than 1,000 × 10 6 / ml have not been reliable for improving wound healing, and most studies have shown that tissue reparative efficacy with PRP can be expected with a minimal increase of five times the normal platelet concentration (approximately) 1 million platelets / μl) [ 13], while much higher concentrations showed no further improvement in wound healing.
The ideal concentration has yet to be defined. The wide variability of platelet concentration devices and techniques used in different studies may alter the degranulation properties of platelets, which may affect clinical outcomes, making interpretation of results difficult.
Components of platelet-rich plasma
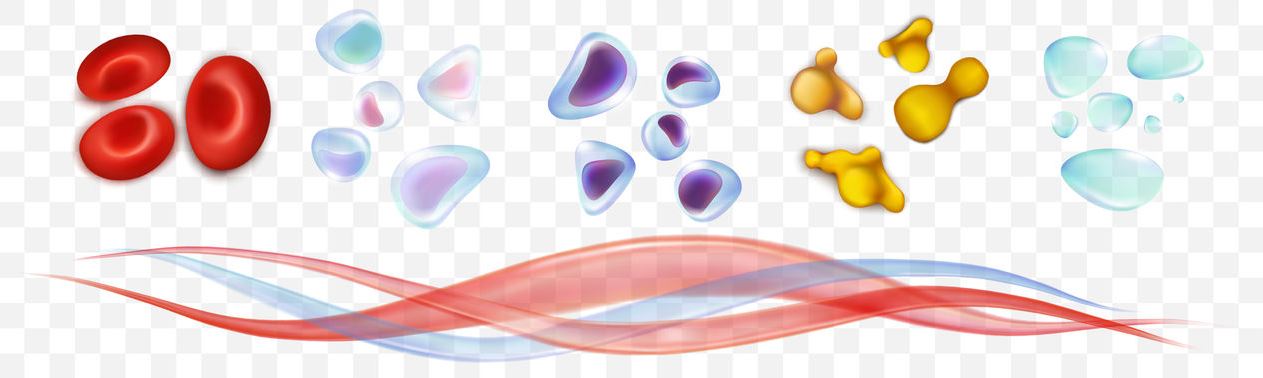
Platelet-rich plasma not only contains platelets, but is also rich in growth factors that are crucial for wound healing:
- Platelet-derived growth factor
- Keratinocyte growth factor
- Interleukin 8
- Vascular endothelial growth factor
- Insulin-like growth factor 1
- Insulin-like growth factor 2
- Connective tissue growth factor
- Fibroblast growth factor
- Transforming growth factor beta
- Epidermal growth factor
PRP also contains blood proteins such as vitronectin, fibronectin and fibrin.
Areas of application of platelet-rich plasma / PRP

There are numerous and ever-growing areas where PRP is being implemented, and its various factions.
- Rheumatology, traumatology or sports medicine
This is certainly the area of greatest projection in the use of PRP, far surpassing even the existing clinical evidence. In vitro PRP has been shown to regulate cytokine processes involved in neovascularisation, proliferation of tenocytes, fibroblasts, myocytes and chondrocytes, and recruitment of inflammatory cells with inhibitory effects of proinflammatory cytokines (IL-1) with anti-inflammatory and regenerative activity.
- Epicondylitis
Epicondylitis is a tendinopathy-limiting condition with a marked tendency to a chronic and incidental partial response to conventional therapy with steroid injections and rehabilitation. Studies with PRP in these patients as a single infiltration resulted in significant functional analgesic improvement and 85% of them resulted in no adverse effect.
- Plantar fasciitis
As with the rest of tendinopathy with a tendency to become chronic, a study of a case series of patients with plantar fasciitis unresponsive to treatment with NSAIDs, immobilisation, physical therapy and corticosteroid infiltration was reviewed with significant functional improvement PRP infiltrated pain in 90% of them.
- Knee osteoarthritis
Case studies of patients compared to single infiltration of hyaluronic acid document up to 35% of respondents to the PRP infiltrate compared to 10% hyaluronic acid. While these studies only cover a small number of patients, it is important to note that for the first time the concentrations of growth factors infiltrated in PRP are specified, emphasising the importance of the leukocyte fraction not potentiating the proinflammatory effect of the final product obtained.
In recent years, the most extensive clinical cases have reported their success in implementing PRP injections. perhaps the largest series of the Spanish, who were part of a group that included the treatment of 261 patients with 3 separate PRP injections of 15 days.
PRP has also been found to be useful in chronic Achilles tendonitis, particularly in infiltrations of ozone, patellar tendinopathy previously used in repair of cuff rotators the anterior cruciate ligament or with plastic erector or tibial tendon graft bone, meniscus repair of the knee joint, in reconstruction of the glenoid labrum or hip and ultimately partial and complete muscle injury here open made later PRP repair and reinforce.
- Foot care
In most cases, the goal of medical research is not only to prolong the life of the patient, but also to improve the quality of the patient. Growth factor rich plasma is a novel and relatively new technique for tissue repair. It consists of a simple system for obtaining platelets and autologous plasma proteins from a patient's blood sample. In the field of podiatry, the use of PRGF enables the improvement of the evolution of patients with regenerative needs in the lower extremities such as: Acceleration of ossification postoperatively, Reduction of resolution time in diabetic ulcers or Improvement of scar formation among many others. Several studies on the use of growth factors have shown excellent results in various medical specialties, among which podiatry.
- Dentistry and maxillofacial surgery
Platelet-rich plasma (PRP) is a new approach to tissue regeneration and is becoming a valuable tool to promote healing in many dental and oral surgery procedures, especially in ageing patients.
- Aggressive periodontitis
Aggressive periodontitis is characterised by rapid loss of attachment, bone destruction and familial aggregation. Platelet-rich plasma (PRP) can help to promote regeneration of lost periodontal tissue.
Platelet-rich plasma has emerged as an alternative in periodontal therapy. PRP appears to increase the speed of the healing process as it is biologically possible that due to the higher concentration of platelets, it can aid wound healing and trigger a faster cellular response than the normal blood clot.
- Dental implants
PRP therapy can be very helpful for dental implants. This includes bone grafting to restore missing bone mass, ridge augmentation and sinus grafting, as well as the actual placement of your dental implants.
After bone grafting, PRP can help regenerate new bone while the surgical incisions heal. After implant placement, PRP helps your soft tissues to heal around your implants while supporting the process of osseointegration.
- Periodontology
Periodontitis is defined as a complex, multifactorial disease characterised by loss of connective tissue attachment with destruction of periodontal tissue. The aim of periodontal therapy is to eliminate inflammatory processes, prevent the progression of periodontitis and also regenerate the lost periodontal tissue.
Platelets play a key role in wound healing and therefore wound healing after periodontal treatment can be accelerated by the use of platelet concentrates . The wound healing process triggered by the formation of blood clots and after tissue injury in periodontal surgery causes platelets to adhere and aggregate, which promotes the formation of thrombin and fibrin . In addition, certain substances are released from platelets that promote tissue repair, angiogenesis , inflammation and immune response .
Platelets also contain biologically active proteins and the binding of these secreted proteins within a developing fibrin network or to the extracellular matrixcan produce chemotactic gradients that favour stem cell recruitment, stimulate cell migration, differentiate and promote repair. Therefore, the use of autologous platelet concentrates is a promising application in the field of periodontal regeneration and can be used in clinical situations requiring rapid healing.
- Gynaecology
PRP is used in gynaecology under the following conditions:
Wound healing:
The use of PRP has been shown to accelerate the healing of surgical wounds and reduce the length of hospital stay, even in high-risk patients such as those with diabetes mellitus. The need for painkillers is also reduced.
Vulval lesions / cervical ectopy:
PRP has been tried for many dermatological and autoimmune diseases of the vulva such as lichen sclerosis, which cause severe itching, dyspareunia and bleeding problems. Almost all patients treated with PRP show improvement. PRP has also been shown to be as effective as laser in treating patients with cervical ectopia with fewer complications such as infection or bleeding.
PRP for genital prolapse and genital fistula:
A study has shown that in patients with small genital fistula, conservative therapy with PRP injection was very successful. The ability of PRP to restore the anatomy and function of the pelvic ligaments is also helpful in women with genital prolapse, especially in the early stages.
PRP in reproductive medicine:
There are promising results in women with premature ovarian failure treated with PRP injection into the ovaries under ultrasound guidance. However, this modality is when the treatment is still in clinical trials and is not a routine treatment. The study was also very promising that injecting PRP into the endometrium can help improve embryo implantation rates in IVF cases.
PRP in gynaecology treatment:
PRP injection into the vagina rejuvenates and regenerates the mucosa, muscles and skin as well as vaginal vascularity. This will result in a greater increase in sensitivity and dramatically improve sexual life. The surrounding skin also becomes thicker and earlier, making the vagina and vulva pinker and more youthful. The ligaments and muscles become stronger, alleviating the problem of urinary incontinence.
- Cardiovascular surgery
PRP has been used in a number of surgical applications (plastic, maxillofacial and orthopaedic surgery) to promote wound and tissue healing. In addition, Staphylococcus aureus, the most common bacterium responsible for DSWI, may be inhibited by the use of PRP.
The use of PRP could also prevent the risk of the patient's body rejecting the foreign transfusion. In addition, surgeons could use PRP at the site where they took the vein for the bypass procedure.
- Plastic surgery
The use of platelet-rich plasma has emerged as one of the most desired non-surgical treatments for facial rejuvenation and hair restoration. It has evolved into a variety of applications in the field of plastic surgery, including its use in combination with microneedling, laser and fat grafting procedures.
Platelet-rich plasma has many properties that make it very attractive for use in plastic surgery: It is easily and inexpensively produced using the patient's own cells, with little or no risk of side effects. However, especially for cosmetic procedures, treatments can be time-consuming and require several sessions.
PRP was originally used to treat skin conditions and to promote bone grafting, and has found a growing number of applications in various surgical specialties - including plastic surgery. In the US alone, plastic surgeons performed more than 130,000 minimally invasive cosmetic procedures in 2019.
PRP has emerged as one of the most desired non-surgical treatments for a number of different cosmetic procedures - although in some cases the claims may outweigh the available evidence. Plastic surgeons are leading the way in identifying promising applications for PRP - including developing standardised procedures and building a body of evidence for good patient outcomes.
- Ophthalmology
The autologous serum shows properties very similar to tears, such as pH, osmolarity, vitamin A and immunoglobulin A. It also shows that tears have several individually distinct components, such as albumin, lactoferrin, lysozymes, aldolase, amylase, fibronectin and substance.
Tears and serum contain abundant common growth factors and antibacterial components that enable the nutritional factors necessary to maintain cell viability in the epithelial repair process.
The use of autologous serum was first described in the search for a lubricious eye drop without harmful preservatives. Later, it became apparent that it could also have true epitheliotrophic potential due to the presence of growth factors and vitamins. Thus, the serum was used as a novel therapeutic approach for ocular surface disorders such as persistent epithelial defects or severe dry eye, which is not treatable with conventional therapy.
Autologous serum has been described not only as a lubricant of the ocular surface, but also as a supplier of various substances essential for the reconstruction of epithelial damage, including vitamin A, epithelial growth factor, fibronectin and various cytokines. With these epitheliotrophic factors, the serum promotes proliferation, migration and differentiation of the ocular surface epithelium. In addition, it is known for its anti-catabolic properties by inhibiting the inflammatory cascade triggered by interleukin-1 (IL-1 ) when it binds to its receptors, preventing tissue destruction.
Therefore, this product has been shown to be effective in the treatment of persistent epithelial defects, neurotrophic ulcers, superior limbal keratoconjunctivitis and dry eye diseases such as graft-versus-host disease or following refractive surgery such as LASIK (laser assisted in situ keratomilesius).
Autologous serum and platelet concentrate have a similar composition as they contain different growth and healing factors present in the blood. However, the autologous serum contains proinflammatory cytokines derived from leukocytes and monocytes, which can be harmful for patients with immunological disorders or diseases.
So, the platelet concentrate has the advantage of not containing these immunoglobulins of inflammation and also regulates the expression of various genes in cellular communication and differentiation, which improves the biological activity of corneal epithelial cells compared to autologous serum.
In addition, PC becomes more effective when it presents higher indices of growth factors, such as: EGF (epithelial growth factor), vitamin A, neuronal growth factor (NGF), insulin type I growth factor and platelet factor IV.
In 2016, Ribeiro et al. also demonstrated how the factors mimic the physicochemical properties of natural tears,(31) which was also demonstrated by Quinto et al. in terms of their importance for corneal and conjunctival epithelial stability and their mechanical and lubricating properties, as well as epitheliotropic and antimicrobial effects.
Growth factors are present in high concentrations in PRP as anabolic agents to support or enhance the healing of damaged tissue, as they are proteins that play an essential role in tissue repair and regeneration processes.
- Dermatology
Platelet-rich plasma (PRP) is an autologous serum containing high concentrations of platelets and growth factors. PRP continues to develop as an important treatment modality with many applications in dermatology, particularly in the areas of hair restoration, skin rejuvenation, acne scars, skin augmentation and striae distensae. In addition, the combination of PRP with laser therapies, microneedling, dermal fillers and autologous fat grafting results in synergistic effects leading to improved aesthetic outcomes. Future studies should standardise PRP treatment protocols for specific indications. PRP shows promise in dermatology as therapeutic applications continue to increase.
- Neurology and neurosurgery
PRP therapy for neurological problems may not be one of the traditional and well-known treatment options, but can be used in patients suffering from some typically difficult-to-treat chronic neurological disorders , peripheral and central nervous system disorders, spinal disorders, etc. . PRP procedures have been shown to be particularly effective in treating the following symptoms and disorders:
- Intercostal neuralgia, lumbago & osteochondrosis
- Ankylosing spondylitis ( Bekhetever's disease)
- Spinal artery syndrome & cervicogenic headaches
- Spinal compression fractures
- Spinal injuries
- Headaches and neck pain
- Spondylarthrosis and spondylosis of the spine
- Herniated and slipped discs
- Kyphoscoliosis & scoliosis
The cause of many neurological diseases is often triggered by inflammation of the spine. Unlike most other parts of the body, the blood supply to the spine is quite poor. As a result, even minor and seemingly treatable neurological problems cannot really benefit from the healing properties of platelet-rich plasma (PRP) - a precious fragment of our blood can help the body heal itself.
Is PRP therapy safe?
Since PRP is only taken from the patient's own blood, complications after the procedure are rarely reported, making this new generation treatment incredibly risk-free. The solution injected into the patient usually contains only platelet-rich plasma. Sometimes medical experts use thixotropic gel and anticoagulants, such as those contained in the PRP tube, to give their patients a more successful PRP treatment.
PRP therapy is an ideal solution for patients who have a low tolerance to certain medications or are prone to allergic reactions.
The results after a PRP therapy session are permanent and can usually last up to 6 months after treatment. This is especially true for treatments with Plasma Fresh, as this product has established itself as the market leader in this niche. Neurological doctors may decide to schedule additional treatments depending on the condition they are treating and its severity.
Related links
Current clinical applications of platelet-rich plasma in various gynecological disorders: An appraisal of theory and practice
Related topics

PRP Tubes and Centrifuges: Compatibility, Best Settings and PRP Protocol
The right combination of PRP tube and centrifuge is crucial for a successful PRP therapy. Our guide will tell you everything you need to know about the compatibility of PRP tubes with common centrifuge models, the best centrifugation settings (RCF, RPM, duration) and tips for maximizing PRP yield. Optimize your treatments with precise settings and high-quality equipment!
Read more
PRP hair growth tubes: how the therapy works
PRP hair growth tubes offer an innovative solution for hair loss. The combination of PRP with melatonin stimulates hair growth, prolongs the growth phase of hair and protects hair follicles from damage. Discover how this therapy works and how it is effectively used to combat hair loss.
Read more
How do I choose the best PRP tubes for my practice?
Choosing the right PRP tubes is crucial to the success of your PRP therapy. Our guide tells you what to look out for: material, certifications, compatibility with centrifuges and costs. Optimize your treatment results with high-quality tubes that offer maximum platelet concentration and purity. Perfect for doctors and clinics that want to integrate PRP into their practice.
Read more
The future of regeneration: PRP and biomimetic peptides – A revolutionary combination
Discover how the combination of platelet-rich plasma (PRP) and biomimetic peptides could transform regenerative medicine. This innovative symbiosis uses the body's natural healing powers and enhances them through targeted cell communication – ideal for aesthetic treatments, wound healing and orthopaedic applications. A glimpse into the future of personalized medicine!
Read more
The future of wound healing: How PRP and silver nanoparticles could revolutionize medicine
Chronic wounds, infections and antibiotic resistance pose immense challenges for modern medicine. But what if we could combine the regenerative powers of PRP (platelet-rich plasma) with the antimicrobial power of silver nanoparticles? This article highlights a groundbreaking idea that combines cell regeneration and infection control. Find out why this innovative combination has the potential to revolutionize wound treatment and dermatology!
Read more
PRP and temporomandibular joint disorders (TMD): A new treatment perspective?
The use of PRP for temporomandibular joint disorders could represent a new treatment option. How does this therapy work and what do the latest studies say?
Read more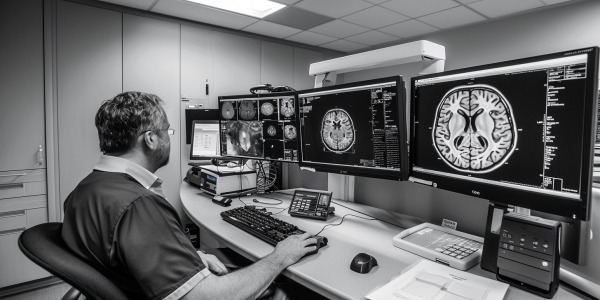
PRP and neuroregeneration: potential for strokes and neurological diseases
The use of PRP in neurological diseases such as strokes is an exciting field of research. What progress has been made in neuroregeneration?
Read more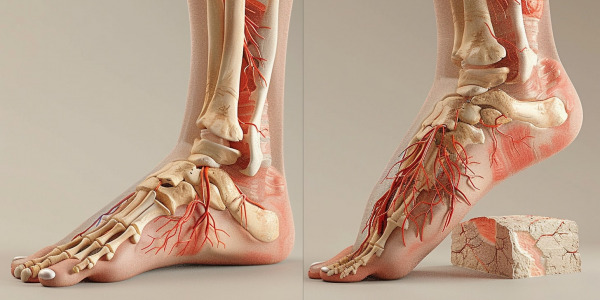
PRP in podiatry: treatment of heel spurs and foot pain
More and more podiatrists are using PRP to treat heel spurs and chronic foot pain. What are the latest findings in this area?
Read more
Dyspareunia-PRP quality of life: a comprehensive overview
Discover how PRP therapy relieves dyspareunia and improves quality of life. Learn more about symptoms, treatments and patient experiences.
Read more
Endometrial problems and the revolutionary role of PRP treatment.
Endometrial problems can be a challenge for women trying to conceive, with thin endometrium posing a particular difficulty. PRP treatment, a method that uses platelet-rich plasma from the patient's own blood, shows promising results in treating endometrial problems.
Read more
Ovarian Insufficiency and PRP Therapy
PRP therapy is a relatively new treatment option for ovarian insufficiency. In this therapy, the body is injected with an autologous plasma preparation enriched with a high concentration of growth factors. These growth factors can stimulate the ovaries and improve egg production.
Read more
Restoration of tubal function with platelet rich plasma
In recent years, the use of PRP to improve ovarian function in women with premature ovarian failure or low ovarian reserve has also been explored. The results of some studies suggest that PRP can increase the number and quality of eggs and improve pregnancy rates.
Read more
Dermaroller and its application: synergies with PRP, serums and hyaluronic acid.
Dermaroller is specifically designed to stimulate the natural regeneration of the skin and is increasingly used in combination with other treatments such as PRP, serums and hyaluronic acid.
Read more
FAQ - PRP training in the areas of trichology, orthopedics and aesthetics.
PRP training in the areas of trichology, orthopedics, and aesthetics is a hands-on, limited time, small group training that specializes in the application of PRP in these areas.
Read more
Your blood. Your power. PRP Penile Injection.
In our latest blog article, we highlight the innovative possibilities of PRP penile injections. What's behind the platelet-rich plasma trend, and how can it help men improve their sexual function? In addition to a detailed look at the procedure and potential benefits of the treatment, we also address potential risks and side effects.
Read more
Applications of PRP in animals: An overview
In this article, we will provide an overview of the applications of PRP in animals and how it can help improve their health.
Read more
Why are platelets of interest to dermatologists?
Platelets are small, seedless blood platelets that play an important role in blood clotting. They can be involved in various skin diseases such as wounds, inflammation or bleeding.
Read more
Required equipment and consumables for PRP treatment
A PRP treatment requires special equipment and consumables. These include a centrifuge, tubes, syringes and needles.
Read more
Lipolysis treatment: A modern way to the dream figure.
Welcome to our comprehensive guide to lipolysis treatment. Are you looking for an effective, minimally invasive method of fat reduction? Then you might be in the right place.
Read more
PRP training: practice upgrade?
The increasing popularity of natural methods of aesthetic medicine has led to the increased use of platelet-rich plasma (PRP). Aesthetic medicine specialists can broaden their horizons and enhance their practice with PRP training. This blog post addresses the benefits of such PRP training.
Read more
PRP aesthetics for men
PRP (platelet-rich plasma) aesthetics is an up-and-coming aesthetic treatment that is becoming increasingly popular, especially among men. In this article, we take a closer look at this innovative method and why it's ideal for men.
Read more
PRP treatments in veterinary medicine: a promising prospect for the future
Platelet rich plasma (PRP) treatments are a promising future prospect in veterinary medicine. Platelet therapy has been established in both veterinary and human medicine for the treatment of poorly perfused tissues.
Read more
Autologous blood therapy for hair
Autologous blood therapy is an innovative and safe treatment method that is becoming increasingly popular for hair loss and thinning hair.
Read more
Can PRP be combined with biorevitalization?
Are PRP and biorevitalization compatible with each other? The preparations act on different processes in the body and complement each other perfectly.
Read more
PRP injections for lips
A PRP treatment for lips consists of a painless injection of platelet-enriched plasma into the skin. The resource for the procedure is the patient's blood, from which platelets are obtained in a concentrated form. These are responsible for stimulating cellular functions and inhibiting the aging process.
Read more
Questions and answers about carboxytherapy
The main cause of aging of the epidermis is a lack of oxygen in the tissues.
Read more
Answers to frequently asked questions about PRP treatment
What is PRP treatment? It is a medical technology that uses an injectable form of autoplasm derived from blood platelets.
Read more
PRP therapy: its therapeutic properties
PRP therapy is an injectable procedure in which a patient's platelet-rich plasma is injected into a body part that requires rapid healing, i.e., it is intended to accelerate regeneration and stimulate the growth of the body's own cells.
Read more
Saving Lives: Blood Plasma
Blood plasma is a versatile drug with pronounced detoxifying and hemostatic properties. It has various functions (nutrition, transport, buffering and others).
Read more
PRP nebulizer for lung diseases - an innovative treatment method
One of the most serious effects of coronavirus disease (COVID19) is lung diseases such as acute respiratory distress syndrome. In the absence of effective treatments, it is necessary to search for new therapies and therapeutic targets. Platelets play a fundamental role in respiratory diseases derived from viral infections, as they are the first line of defense against viruses and are essential for maintaining lung function.
Read more
What is regenerative medicine?
Regenerative medicine encompasses many different innovative therapies whose goal is autologous (the body's own) tissue regeneration.
Read more
PRP treatment in sports medicine
PRP is an agent used to biologically stimulate tissue healing. It can be an effective method of treating sports injuries and is therefore becoming increasingly popular. PRP procedure can and should play an important role in solving the most current orthopedic problems in the present and in the future!
Read more
PRP treatment for rosacea
PPR allows the skin to rejuvenate and repair itself, which can help relieve and calm the symptoms of rosacea.
Read moreTreatment of cellulite with PRP (platelet rich plasma)
In the modern world, 90% of women struggle with body blemishes (cellulite, stretch marks). The introduction of autologous platelet plasma can reduce the severity of these defects and improve the quality and appearance of the skin.
Read moreHair Loss Support and Treatment
Hair loss, also called alopecia, is complete or partial baldness due to hormonal changes or physical or psychological stress.
Read more
FUE hair transplantation
FUE transplants are the most common and successful method of curing hair loss. Find out more about the FUE hair transplant process.
Read more
You want to make plasma gel? What equipment do you need to do this?
We are often asked what equipment is needed for plasma gel? You will find an answer in this article.
Read morePlasma growth factors in cerebral palsy
The use of plasma growth factors has opened up a new clinical field of application in medicine and given rise to a new discipline called regenerative medicine. In many areas such as traumatology, dental implants or anaesthesia, the use of this biotechnology can improve patients' quality of life.
Read more
PRP therapy for tendonitis
Repetitive movements can stretch tendons and cause pain, swelling and limited movement. Try PRP therapy to perform tendon repair, which can heal hard tissue and not just mask pain and cause long-term damage like traditional treatments.
Read moreLearn more about PRP treatment: how it works and what it does.
PRP treatments are an innovative technique that helps improve skin quality and treat certain skin conditions. These treatments are safe, gentle and effective and can help improve the appearance and condition of the skin. Learn more about PRP treatments, how they work, and what results you can expect.
Read moreCan carpal tunnel syndrome be treated with PRP therapy?
Carpal tunnel syndrome (CTS) is a condition that affects a patient's quality of life. About three to six percent of the adult population in the United States suffers from carpal tunnel. Some cases of CTS improve on their own, but many require medical intervention. Unfortunately, many modern medical treatments offer only short-term relief for patients. They do not solve the underlying problem that causes CTS.
Read morePRP or dermal filler - Which should I choose?
People of all ages are concerned with combating various signs of skin ageing. Some of the most popular options for patients are injectables such as dermal fillers and platelet-rich plasma injections. These two are non-surgical enhancement techniques that help you look younger than your actual age.
Read morePRP treatment after hair transplantation
PRP treatment after hair transplantation is used to promote faster wound healing and hair growth after hair transplantation. PRP treatment is said to help revitalise weak hair follicles that are prone to falling out. It has been observed that the hair in the treated area is less thin and the hair shafts are thicker in patients treated with PRP.
Read moreWhat is the effect of PRP therapy in orthopaedics?
In recent years, various methods of using platelet-rich plasma (PRP) have been applied during the treatment of various orthopaedic diseases and sports traumas. They enable the improvement of the local biological condition and the regeneration of different tissue types. PRP is a modern treatment strategy with worldwide recognition.
Read morePlatelet-rich plasma: the key to PRP therapy
Platelet-rich plasma (PRP) is used in a variety of clinical applications based on the premise that higher GF content should promote better healing. Platelet derivatives represent a promising therapeutic modality and offer possibilities for the treatment of wounds, ulcers, soft tissue injuries and various other cell therapy applications.
Read moreDoes PRP treatment work for hair loss?
Platelet-rich plasma (PRP) is a treatment that doctors use to speed up healing in different areas of the body. It can help restore hair growth. Doctors usually use this treatment for hair loss results from androgenetic alopecia, a common condition that causes hair follicles to shrink.
Read morePRP treatment against melasma
There is no shortage of treatments to "cure" melasma, but unfortunately many of them do not work and simply rob clients of time, money and emotional stress. Platelet-rich plasma (PRP), however, offers promising treatment options for people living with melasma. Let's first discuss the disease and how PRP can help with the condition.
Read more
What are PRP tubes?
Platelet-rich plasma, better known as PRP, is an autologous procedure in which a person's whole blood is drawn. The platelets are then concentrated using a centrifuge and special PRP tubes. The platelets, which contain several growth factors, are then taken again -in this feature injected into the same person makes PRP alone a very safe procedure that eliminates the likelihood of contracting communicable diseases.
Read morePhotodynamic therapy (PDT)
Photodynamic therapy (PDT) is a treatment that involves light-sensitive drugs and a light source to destroy abnormal cells. It can be used to treat some skin and eye diseases as well as certain types of cancer .
Read moreLipogems / Lipogems Treatment
Lipogems is a medical device that extracts fat (also called adipose tissue) from your abdomen and injects it into your arthritic and/or painful joint. This helps relieve joint pain and allows you to regain function and return to your daily activities.
Read morePRP treatment of diabetic foot ulcers and wounds
PRP treatment of diabetic foot ulcer is effective and safe. PRP is effective if it significantly accelerates the healing of the diabetic foot ulcer and safe if it does not cause significant changes in the patient's blood haematology or blood chemistry (albumin).
Read morePRP therapy for back pain
By injecting PRP directly into the lower back, these growth factors and proteins are concentrated exactly where they are needed so they can begin to heal and repair damaged areas to relieve pain and restore normal spinal function.
Read morePlatelet Rich Plasma (PRP) for brain injuries
PRP is rich in numerous growth factors associated with the repair processes following injury to the central nervous system, which consists of the brain and spinal cord.
Read moreThe most common sports injuries that can be treated with PRP.
Many sports injuries improve with platelet-rich plasma (PRP) injections. Both professional athletes and weekend warriors can be out due to injuries. Athletes have traditionally had the choice of either sitting out for weeks or months to heal or undergoing major surgery - neither of which is particularly desirable. PRP injections offer a radical third alternative. This minimally invasive, safe and fast orthobiological treatment is highly effective for many of the most common sports injuries.
Read morePRP in gynaecology - Vaginal rejuvenation
PRP can be extremely beneficial for vaginal rejuvenation. As platelets are responsible for both promoting healing and regenerating healthy tissues in your body, PRP can be an ideal solution if you are looking for a vaginal treatment with rejuvenating properties. Depending on your needs, PRP injections can be performed into the tissues surrounding the clitoris, urethra and G-spot. When injected into the areas targeted for treatment,
Read morePRP treatment for wrist pain
Hands and wrists are amazingly complex, with 27 bones, a complex network of ligaments, tendons, joints, nerves and muscles working gracefully together. The human hand can type across a keyboard, serve a tennis ball, turn a doorknob and feel the gentle touch of a child's hand. If you are suffering from an injury to the ligaments or tendons in your hands, wrists or elbows, a PRP injection can speed up the healing process. Your doctor may use a PRP injection with surgery to help you recover faster.
Read more
Why should you offer PRP injections in your medical practice?
PRP is used in almost every field and specialty, from sports medicine to pain management, skin rejuvenation, hair care and urology. Most doctors who use this treatment also saw higher patient retention rates. So is there a legitimate reason not to add PRP to your practice?
Read morePRP (Platelet Rich Plasma) in cardiac surgery
PRP is a safe, simple and reproducible therapy that appears to offer both clinical and financial benefit to patients undergoing sternotomy for cardiac surgery. The addition of PRP to all sternal occlusions following cardiac surgery brings value by improving care and reducing costs.
Read morePRP (Platelet Rich Plasma) treatment for COPD disorders
PRP treatments for COPD conditions can help repair the air sacs or alveoli and reverse lung damage caused by smoking, pollution and other factors. Make breathing easier, relieve chest discomfort and increase stamina with PRP therapy.
Read more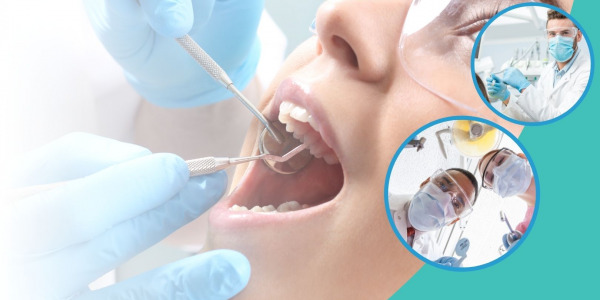
PRP treatment for periodontal disease
Inflammatory periodontal disease is one of the most pressing problems in dentistry, which is not only of general medical but also of social importance.
Read morePRP (Platelet Rich Plasma) therapy in dermatology
Platelet-rich plasma (PRP) is an autologous serum containing high concentrations of platelets and growth factors. PRP therapy continues to evolve as an important treatment modality with many applications in dermatology, particularly in the areas of hair restoration, skin rejuvenation, acne scars, skin augmentation and striae distensae. In addition, the combination of PRP with laser therapies, microneedling, dermal fillers and autologous fat grafting leads to synergistic effects that result in improved aesthetic outcomes.
Read moreUse of PRP (Platelet Rich Plasma) therapy in dogs with pain.
Is your dog recovering from an injury or suffering from degenerative joint disease? Platelet-rich plasma therapy (PRP) can help.
Read more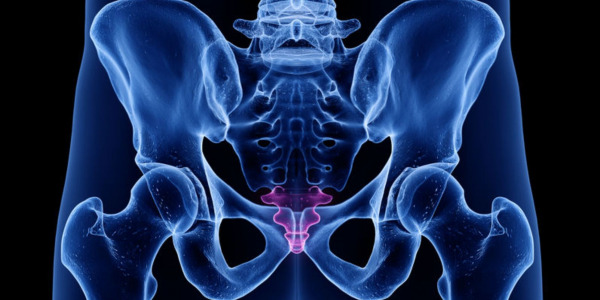
PRP (Platelet Rich Plasma) treatment for coccygodynia
Try PRP for coccydynia or tailbone pain, a condition for which there are no conventional remedies apart from treatments to relieve symptoms. Gain a better quality of life with the ability to sit pain-free and need support.
Read more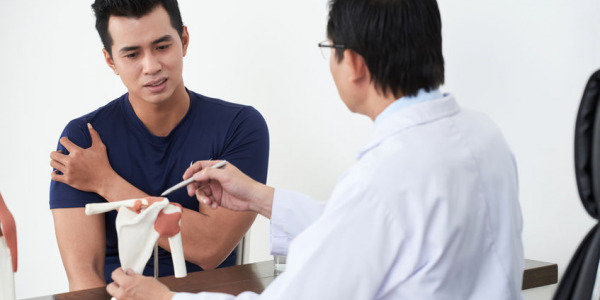
PRP treatment for shoulder pain
In the orthopaedic community, the clinical use of PRP (platelet-rich plasma) in the treatment of shoulder pathologies has increased rapidly over the last decade.
Read more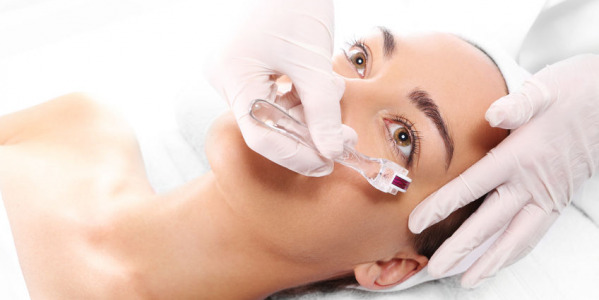
Microneedling for acne scars
As if acne is not frustrating enough, sometimes you have to deal with the scars that acne may leave. Acne scars may appear due to cystic acne or itchy skin. Like other types of scars, acne scars can last for months or longer. Even a few years. Want to learn more about microneedles for acne scars? Read on to learn more about the procedure and discuss its effectiveness and possible side effects with your dermatologist.
Read morePRP (Platelet Rich Plasma) therapy for plantar fasciitis
Recently, platelet-rich plasma (PRP) has been used as an alternative therapy for plantar fasciitis (PF) to relieve heel pain and improve functional recovery.
Read more
What are platelet rich plasma (PRP) injections?
Times have changed since the days of bloodshed, when doctors treated their patients by drawing blood from them. Now a procedure called platelet-rich plasma therapy has emerged in which some of the blood is injected back into a diseased joint. You could say it's bloodshed in reverse.
Read more
Does PRP therapy help with tennis elbow?
Platelet-rich plasma (PRP) therapy uses the body's own natural healing processes to repair damaged tissue. Platelets are blood cells that promote blood clotting and support wound healing. PRP contains many proteins called growth factors (more than normal blood) that help the tendon to heal and consequently relieve your pain.
Read morePRP progress: Why you as a medical professional should offer this treatment.
Platelet-rich plasma (PRP) has received considerable attention in the field of dermatology since the elucidation of its mechanism and reports of its clinical efficacy. PRP alone or in combination with other therapies has shown benefits for some cosmetic problems and skin conditions. Few transient or short-term side effects have been reported with the use of PRP. In this paper we highlight the potential efficacy and benefits of PRP
Read morePRP therapy for eye diseases
Blood products (autologous serum, platelet-rich plasma (E-PRP), plasma rich in growth factors) are successful therapies for ocular surface diseases that affect the integrity of the corneal surface and conjunctiva.
Read more
PRP treatment for knee pain
Does PRP treatment work for knee pain? Platelet-rich plasma (PRP) injections are a novel treatment for pain associated with osteoarthritis of the knee.
Read more
PRP treatment for erectile dysfunction
Platelet-rich plasma (PRP) found its use in the treatment of various conditions and diseases, as concentrated plasma PRP consists of many growth factors. Their interaction with surrounding cells, intracellular matrix and mediators at the injection site leads to tissue regeneration. Angiogenic, vasculogenic and regenerative effects of PRP can be used to treat erectile dysfunction (ED) and Peyronie's disease (PD).
Read more
PRP injection or cortisone injection? - Which is the best option?
Before the development of PRP (platelet-rich plasma) injections, doctors generally used cortisone injections to relieve moderate to severe muscle / joint inflammation and (some) pain. However, with the creation of PRP injections, doctors can now relieve inflammation and pain as well as help the damaged tissue heal.
Read moreThe right care after PRP treatment
If you have PRP therapy applied as a topical serum for skin problems, your doctor will probably recommend no strenuous physical activity or exercise for about 48 to 72 hours after treatment. Recommendations may differ for other PRP applications, including orthopaedic injuries and hair loss. The best way to ensure proper healing and ideal results is to follow your provider's post-operative guidelines closely, including temporarily interrupting your exercise routine if recommended.
Read more
PRP Tubes | Vi PRP-PRO Set
PRP tubes | Vi PRP-PRO set with separating gel and anticoagulant. Platelet-rich plasma (PRP) therapy is an innovative treatment that stimulates the body's natural healing process and utilizes the patient's own cells to promote accelerated healing of certain musculoskeletal disorders, sports injuries and arthritic joints. It provides powerful growth factors that stimulate and enhance the blood supply to the injured area and the nutrients cells need to regenerate damaged tissue.
Read more
Treat dark circles with Vampire Lift / PRP therapy
Injecting the platelet-rich plasma under the eyes gives the skin below the eye the vital nourishment it needs. Once injected into your skin, the platelets promote the growth and regeneration of your own collagen, resulting in increased smoothness and firmness of the skin.
Read morePRP therapy for injury scars
PLATELET GROWTH FACTORS derived from blood (plasma) and responsible for repair processes can regenerate the skin in injury scars. The concentration of platelet growth factors in platelet-rich plasma (PRP) is about 95%, compared to only 4 to 5% found in normal-forming clots. Therefore, PRP can stimulate tissue regeneration much faster than normal.
Read moreWound healing through PRP therapy
Many elements such as cytokines and growth factors are involved in the regeneration process of injured tissues. The growth factors contained in platelets represent an important physiological mixture of factors that may be involved in the healing process.
Read morePRP treatment for acne
Platelet-rich plasma is injected into the acne-damaged area of the face to stimulate the production of new collagen and elastin, reduce the appearance of scars, and make the skin look brighter and smoother.
Read more
Density Platelet Gel - PRP-Tubes
Density Platelet Gel - PRP tubes for your PRP treatments.
Read more
PRP injection for facial beautification
Is platelet-rich plasma the secret to younger-looking skin? What exactly are PRP injections for facial beautification?
Read morePRP skin treatments
The body cells that help tissues heal and produce new cells are called platelets. PRP is injected into specific areas of the skin and then creates an environment that helps with the growth of collagen, regenerates tissue and makes your skin smooth and firm. PRP reduces wrinkles and creates a skin texture and tone that is smoother, younger and better.
Read morePRP treatment for hair loss - questions and answers
PRP therapy for hair loss is also known as platelet-rich plasma therapy . It is a treatment offered to men and women of all ethnicities. It is a simple, non-surgical procedure in which the patient's PRP is extracted by drawing blood and separating the platelet-rich plasma from the rest of the blood using a centrifuge. The plasma is then injected into the thinning areas of the scalp to stimulate hair growth and provide fuller, healthier looking hair.
Read more





